The Anatomy of Neurodivergent Burnout — Part 3
Sensory overload, systemic barriers and the absence of accommodations — the invisible cost of existing in a world not designed for your brain.

Introduction: You Are Not the Problem
There is a persistent narrative, often unspoken yet omnipresent, that goes something like this: if you organised yourself better, if you were more resilient, if you tried just a little harder — you would be fine. This is a story of individual failure. And it is profoundly wrong.
Neurodivergent burnout does not arise because your nervous system is “broken”. It arises because you live in a world not designed for the way you process reality. Research is explicit: autistic burnout is “an environmental problem, not an individual, personal problem or character flaw” — it is the predictable result of a chronic mismatch between external demands and the person’s resources, in the absence of adequate support (Raymaker et al., 2020).
The social-relational model of disability shows us that burnout is not a personal failure — it is the price you pay for functioning within a system that does not include you.
In Parts 1 and 2 we explored the internal mechanics of collapse. Now we complete the picture with the other half of the equation: the external factors that fuel the storm. We will explore three essential dimensions:
1. Sensory overload — how processing works differently and why the “normal” environment is a continuous neurological assault
2. Systemic barriers — how institutions exclude you by design
3. The absence of accommodations — why “take a break” does not work when the system does not allow it
◆ ◆ ◆
What Sensory Overload Is
More than “a preference”: a neurological reality
Sensory overload is not a whim and it is not “sensitivity” in any colloquial sense. It is a state of neurobiological overwhelm — acute or chronic — that arises when the brain receives more sensory information than it can process or integrate effectively.
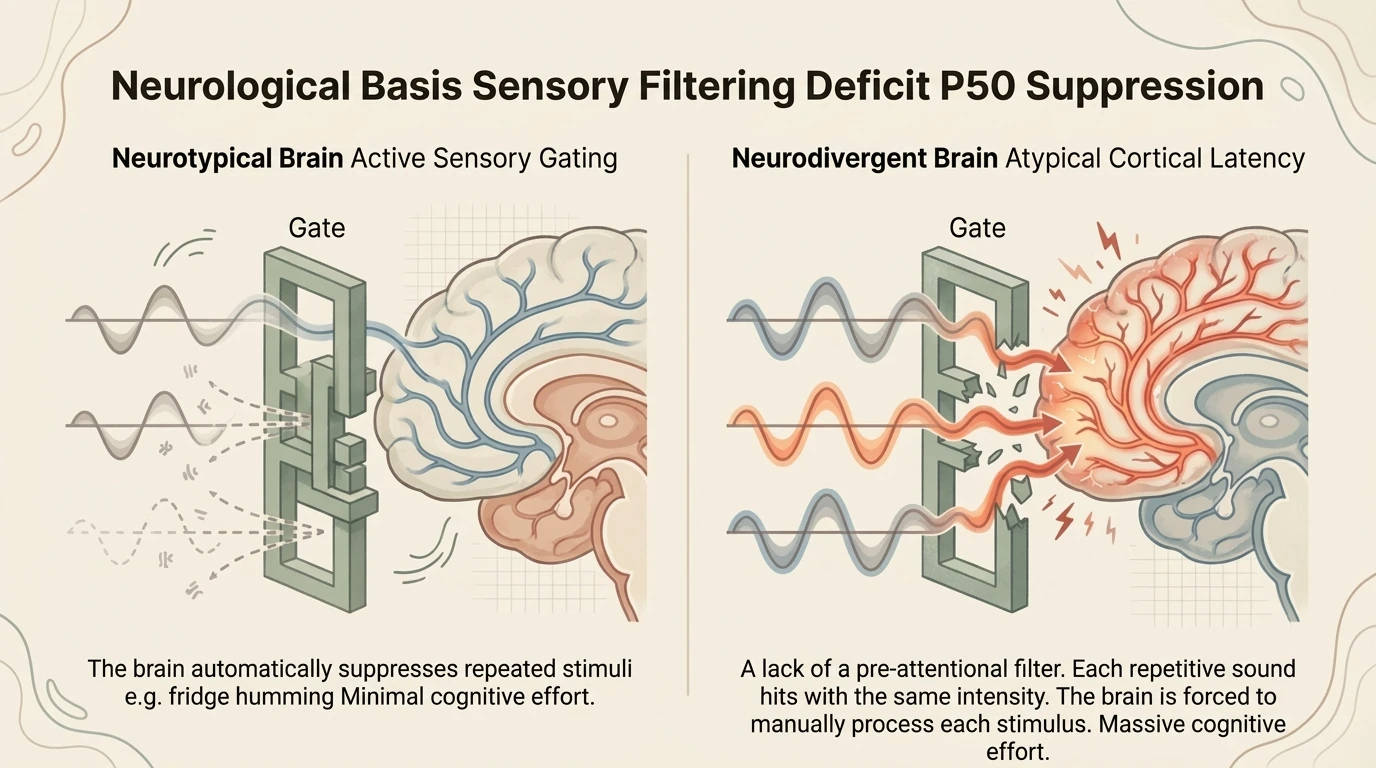
Over 96% of autistic people experience significant sensory processing differences (Marco et al., 2011). We are not talking about a more intense version of the neurotypical experience. We are talking about a nervous system that functions in a fundamentally different way.
The neurotypical brain uses a process called habituation — the capacity to “ignore” repetitive background stimuli. The fridge’s hum, fluorescent lighting, colleagues’ conversations — all are automatically filtered and placed in the background. The neurodivergent brain does not do this. “We don’t filter out and eliminate background sensory information. We receive it all the time, at all hours of the day.”
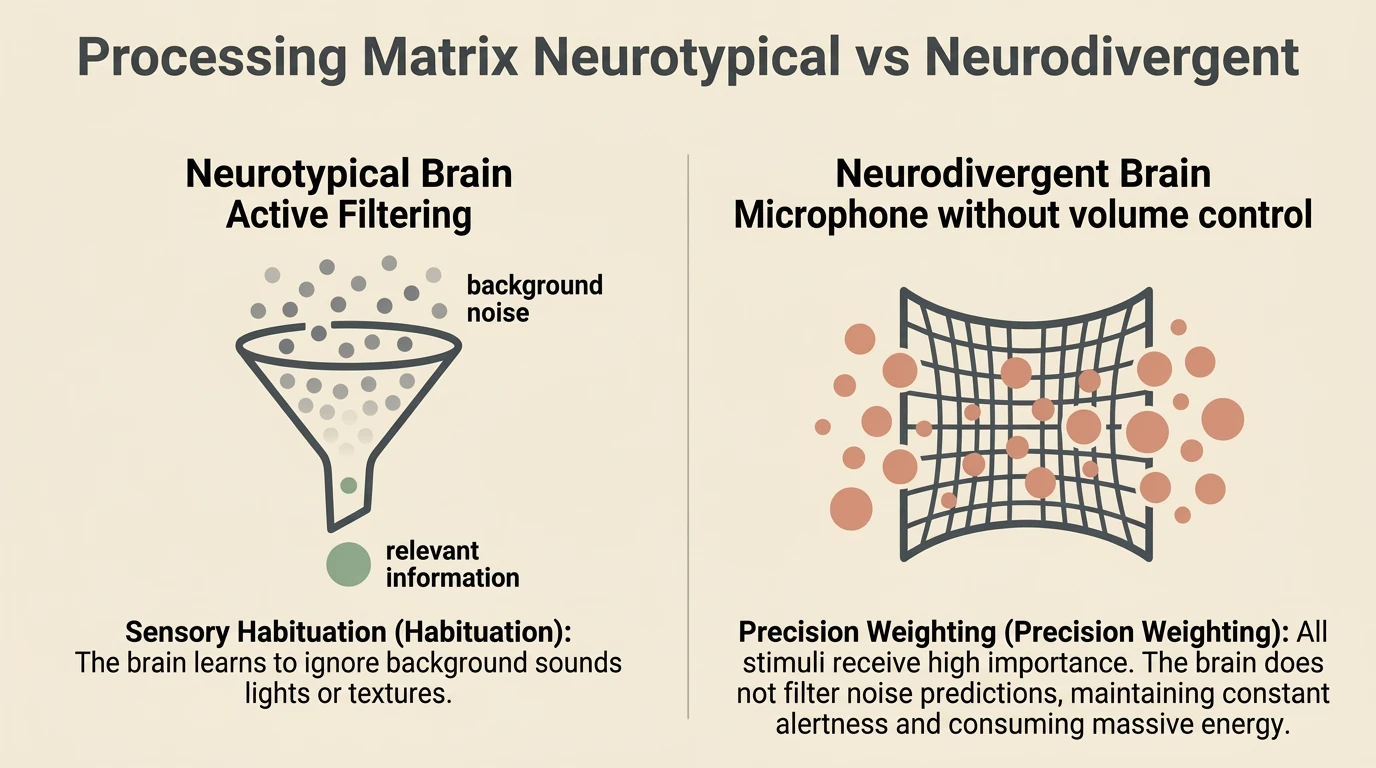
Predictive processing and precision weighting
Recent research offers a neurobiological explanation for this difference. In the predictive processing model, the brain continuously constructs predictions about what it will experience — and pays attention only to deviations from the prediction. In autistic people, this mechanism works differently: the brain assigns a different precision weighting to stimuli. Prediction errors are not filtered out but treated as urgent and vital information. Each repetitive sound is processed as though it were new and relevant.
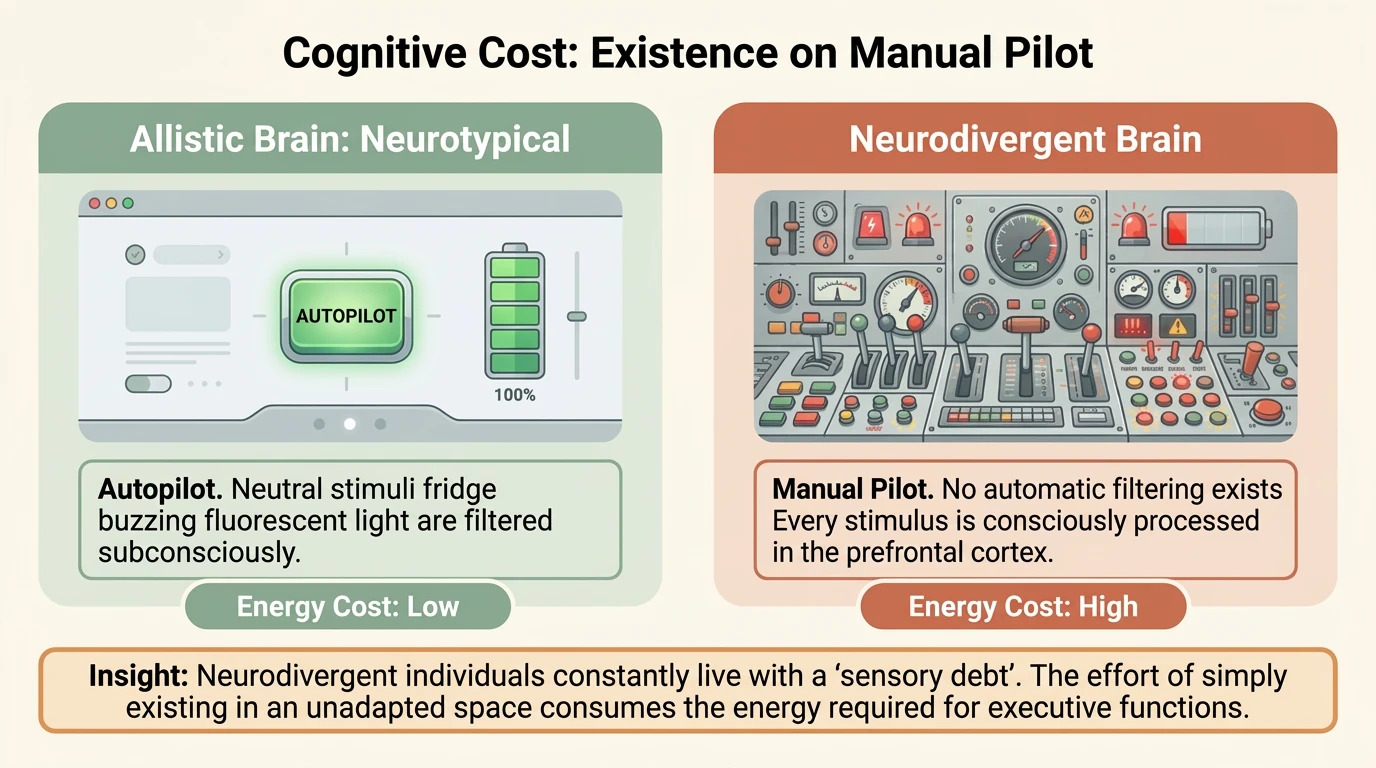
The result? A high-bandwidth processing system that notices details invisible to neurotypical people — but one that consumes significantly more metabolic energy. What for a neurotypical brain is automatic processing — “autopilot” — for the neurodivergent brain is manual emulation: every stimulus processed consciously, in the prefrontal cortex, at maximum energy cost.
◆ ◆ ◆
The Invisible Cost of Daily Existence
When “existing” costs energy
Imagine an ordinary day. You wake up — but not at 100% battery. Because of chronic sleep dysregulation (common in neurodivergent people), you start the day at 60%. The shower: the tactile load of temperature, the textures of clothing — minus 10%. Transit: background noise, crowds, mixed smells — minus 10%. The office: fluorescent lights, simultaneous conversations — minus 10%. The first “simple” social interaction: eye contact, active tone analysis, suppressing a stim — minus 15%. A small act of self-regulation: suppressing the need to rock or leave the room — minus 20%.
It is lunchtime. You have 5% battery. And the day has barely begun.
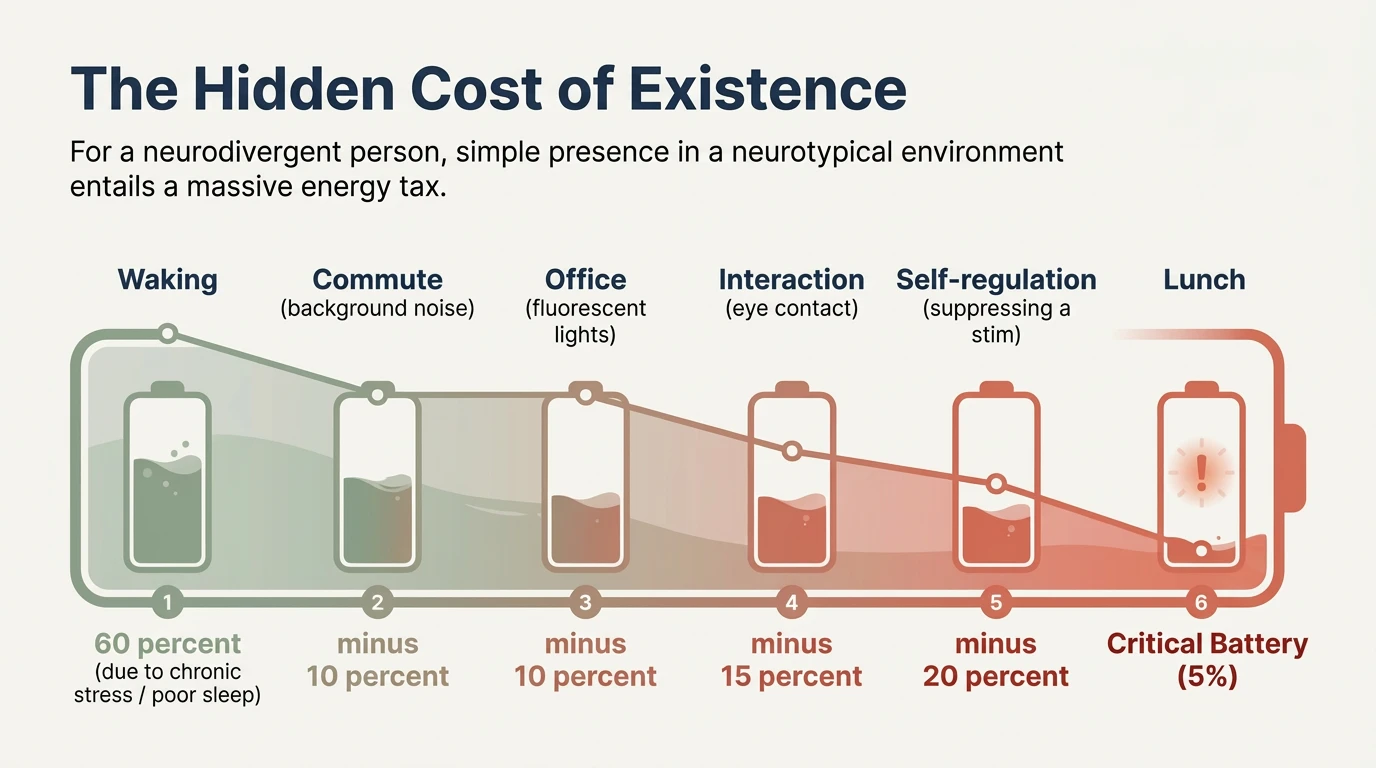
This is not dramatic exaggeration. It is the neurological mathematics of existing in an environment not designed for you. What studies call “allostatic load” — the chronic wear on the nervous system caused by repeated exposure to sensory friction — is for neurodivergent people not an exception but the default daily experience.
The filling cup: the cumulative process
Sensory overload is not a singular event. It is a cumulative process — like a cup filling drop by drop throughout the day. Each stimulus adds a layer: at the base, background noise that cannot be filtered; above it, fluorescent lights; then clothing tags irritating the skin; and at the top, the effort of masking that consumes the last reserves. Masking dramatically accelerates the filling of the cup, because it consumes precisely the cognitive reserves needed for sensory regulation.
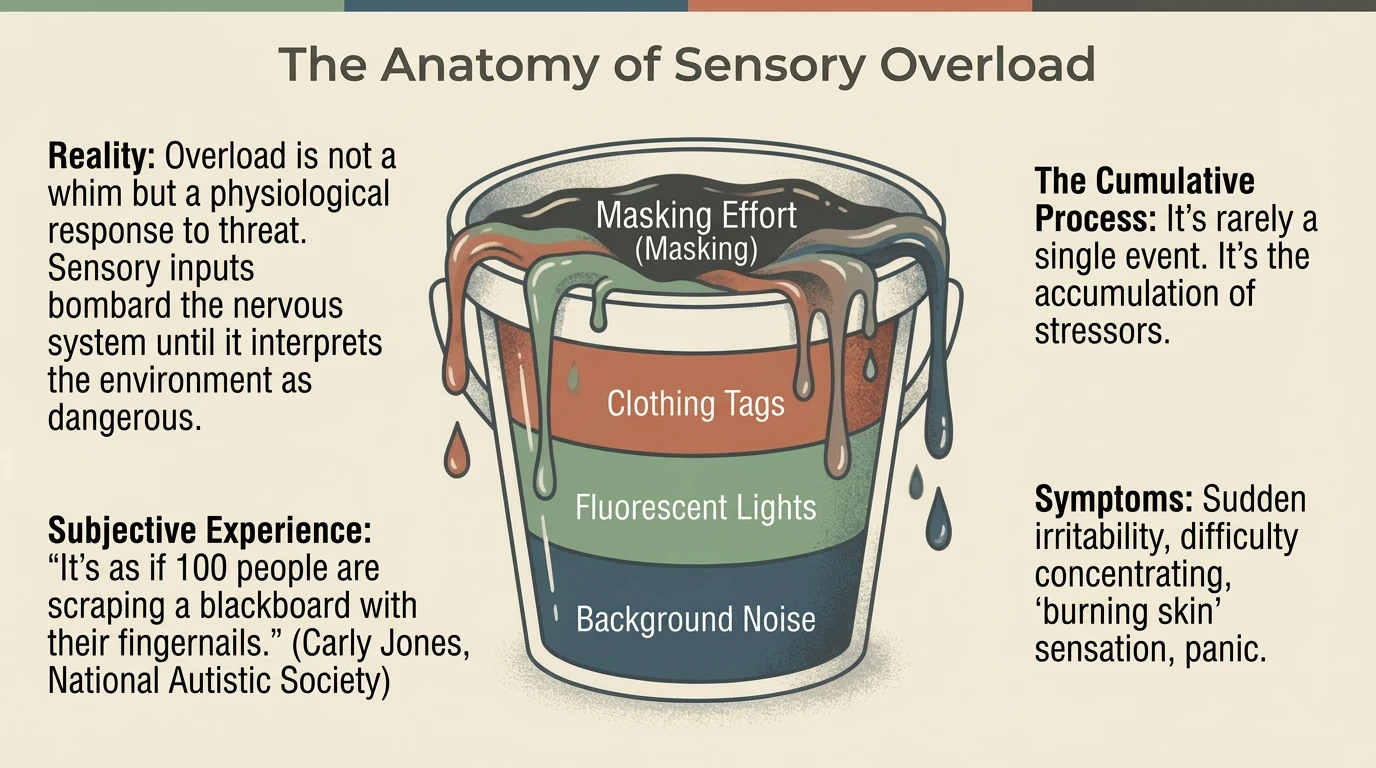
When the cup overflows, the nervous system is bombarded with more information than it can process. The result: a crisis. And importantly — it is an involuntary physiological reaction, not a “temper tantrum” or a behavioural choice.
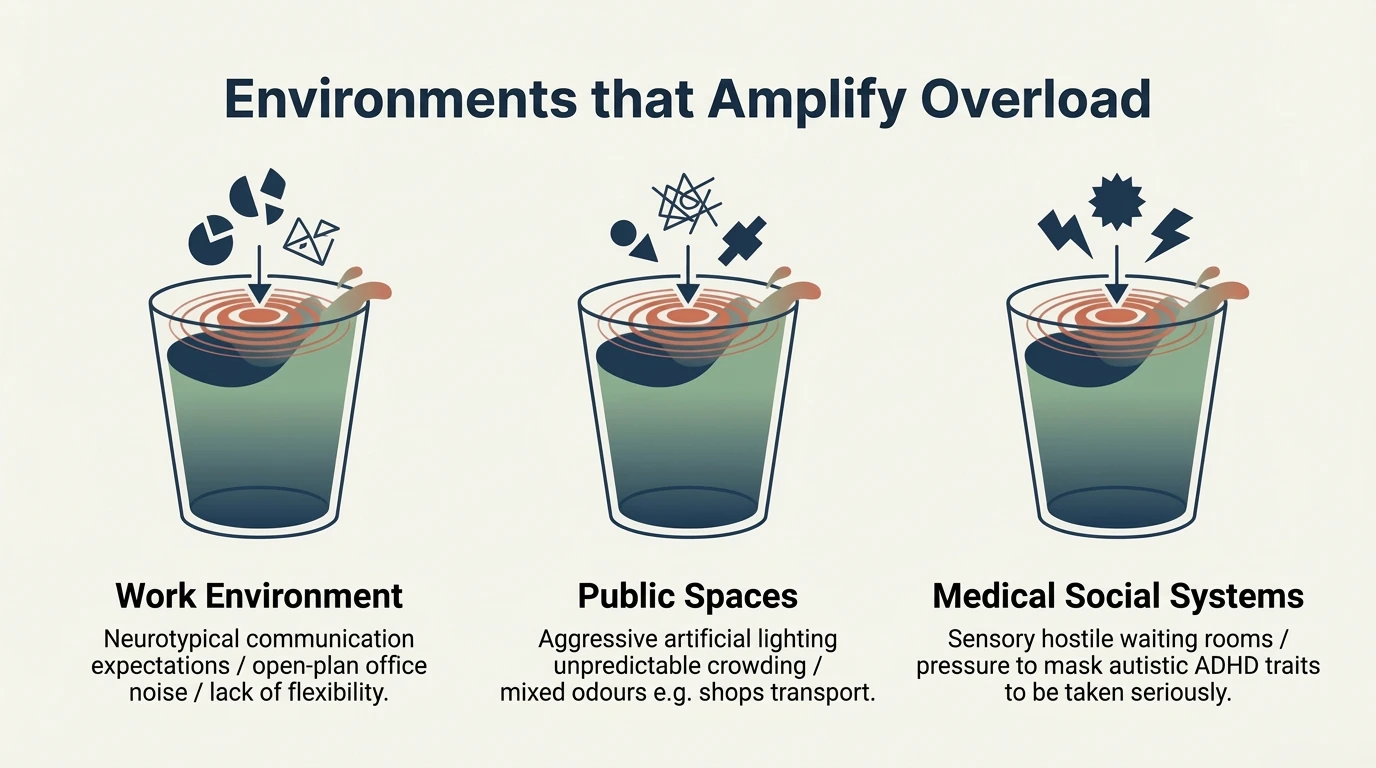
Daily friction: the sensory minefield at work
Now look at the work environment through the lens of neurodivergent sensory processing.
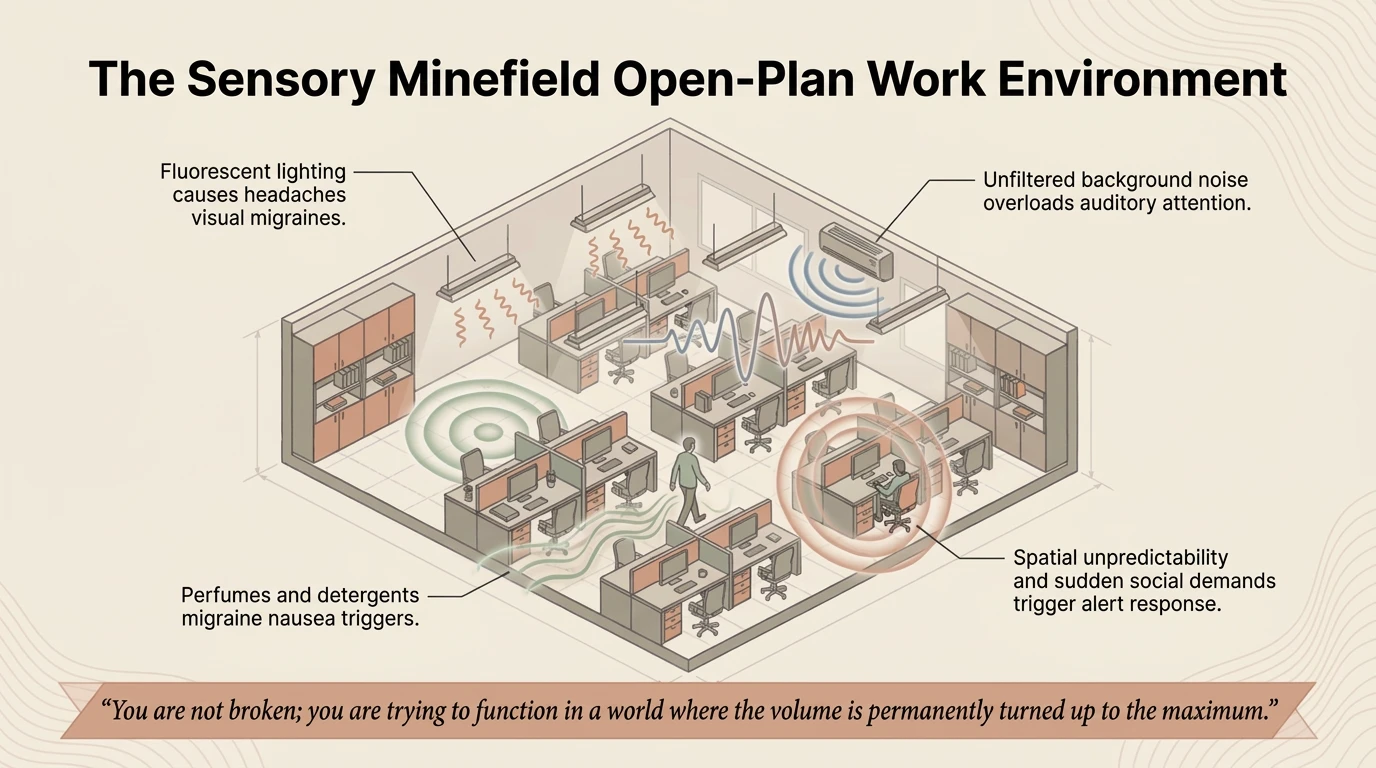
Fluorescent lighting — it flickers constantly, imperceptible to most, painful for the neurodivergent brain. It causes headaches, visual migraines and continuous neurological stress.
Unfiltered background noise — overlapping conversations, keyboards, phones — the brain’s inability to filter speech acoustically. Every conversation is processed at full volume.
Olfactory bombardment — colleagues’ perfumes, cleaning chemicals, the smell of reheated food — processed at maximum intensity, triggering nausea or migraine.
Spatial unpredictability — unannounced meetings, ambiguous verbal instructions, forced eye contact, constant interruptions — trigger the alert response.
What for a neurotypical person is “harmless background”, for a neurodivergent person is an active bombardment.
◆ ◆ ◆
The Exhaustion Feedback Loop
Sensory overload does not stop at daily friction — it self-amplifies. Research describes a four-stage feedback loop that transforms daily friction into collapse:
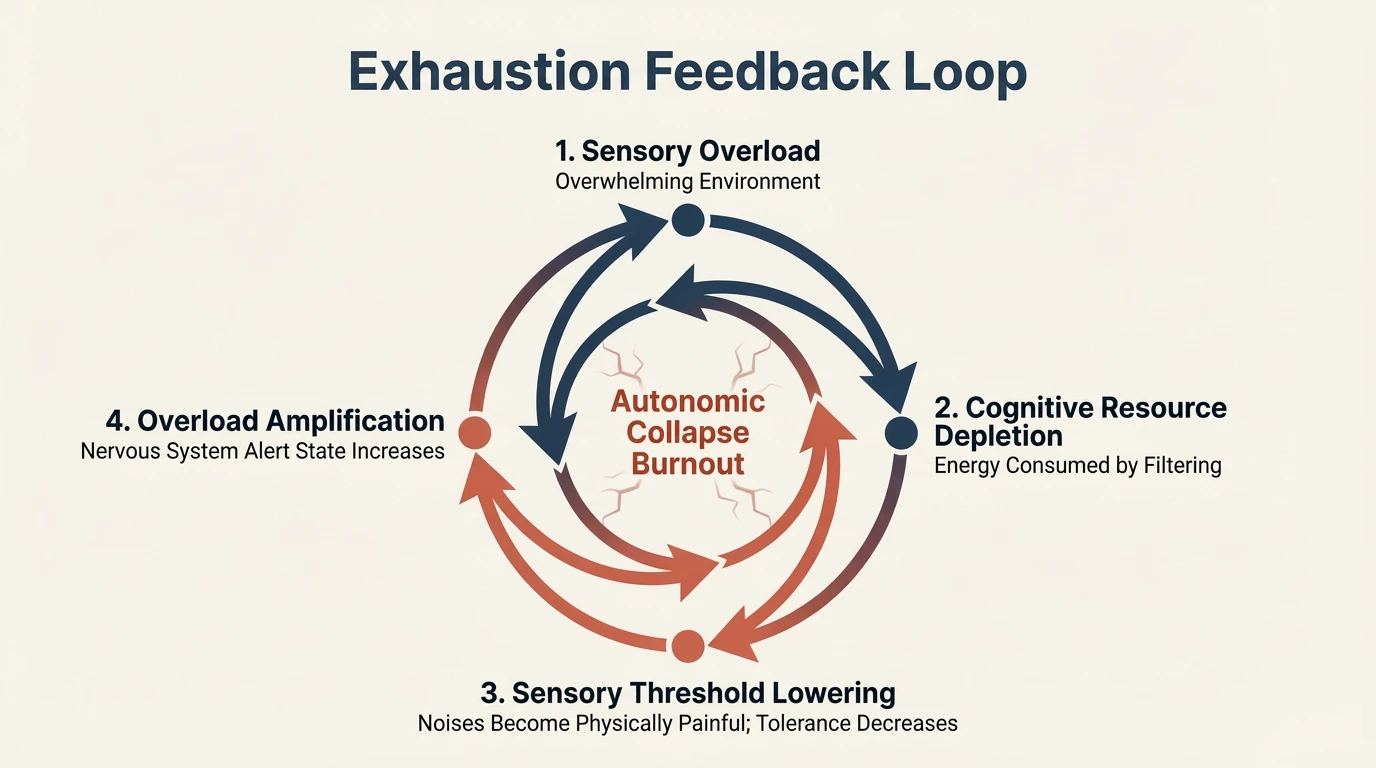
Stage 1 — Sensory overload: An overwhelming environment delivers stimuli the brain cannot filter.
Stage 2 — Depletion of cognitive resources: Energy is consumed by the “manual” processing of each stimulus.
Stage 3 — Lowering of the sensory threshold: The tolerance threshold drops. “A background hum that was previously manageable can become an unbearable and painful noise. A light touch can be perceived as intensely irritating.” Tools that once worked — headphones, quiet rooms, predictable routines — begin to be insufficient.
Stage 4 — Amplification: The nervous system’s state of alert rises, sensitivity intensifies, and the cycle begins again — each time from a lower baseline of resources.
Biologically, studies that have examined autonomic nervous system function in autistic people confirm a distinct profile of elevated baseline hyperactivation: elevated heart rate, lower heart rate variability (HRV) and increased electrodermal activity — the objective signs of an organism living permanently in fight-or-flight mode.
When the system gives way: meltdown and shutdown
When the loop accelerates and resources reach zero, the nervous system takes over. But collapse does not look the same for everyone:

A meltdown is an explosive collapse — a fight/flight response. The overwhelmed nervous system releases accumulated pressure through externalisation: crying, shouting, motor agitation, intense stimming. It is not a “tantrum” and it has no purpose. It is a neurological safety valve.
A shutdown is an implosive collapse — a freeze response. The nervous system disconnects to conserve energy. The person becomes quiet (selective mutism), still, with a “blank” gaze, unable to process language. It can last from minutes to days.
◆ ◆ ◆
Systemic Barriers: When Institutions Exclude You by Design
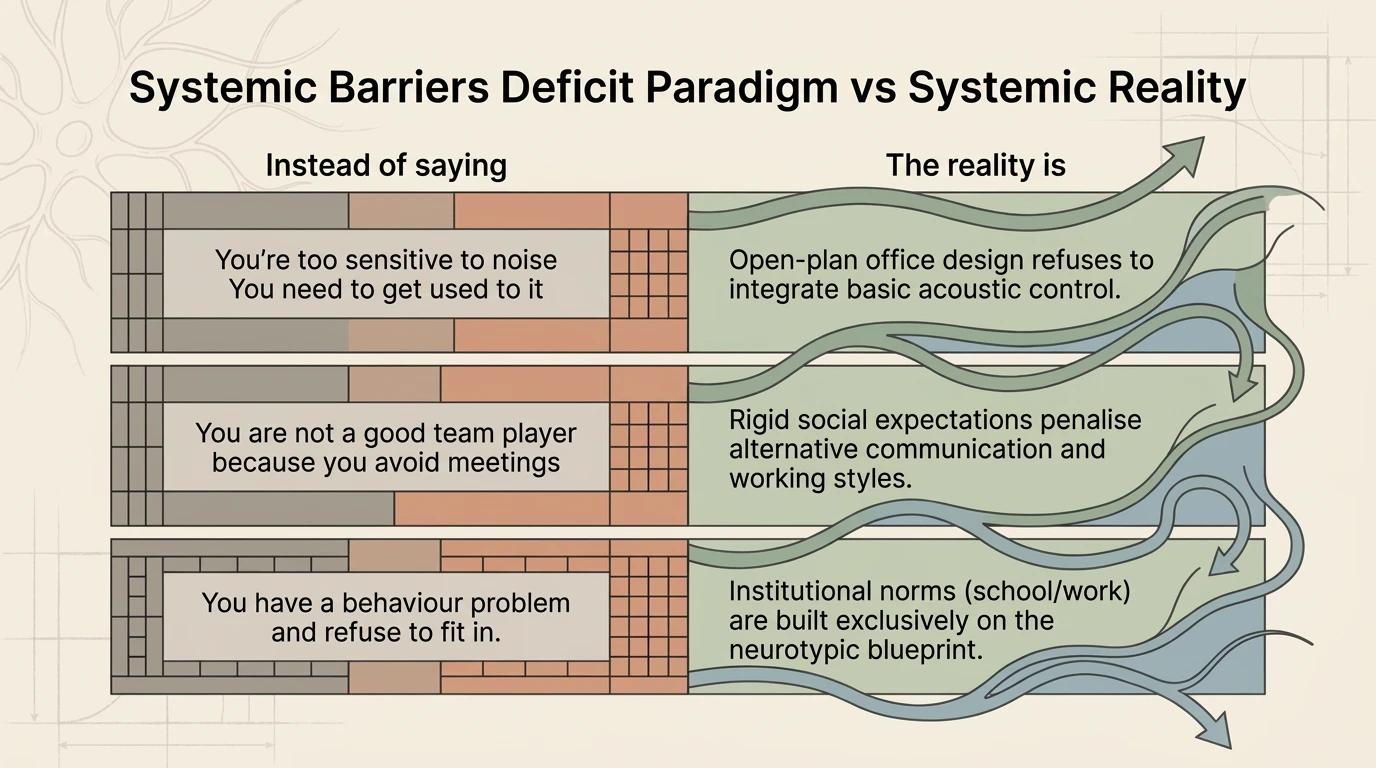
The problems are not only sensory. There are entire structures — at work, in education, in healthcare — built on the assumption that all people function identically. This model is not neutral. It is discriminatory by omission.
And the most damaging aspect: the dominant narrative places the blame on the individual. “You’re too sensitive to noise” — when in fact the open-plan office design refuses to integrate basic acoustic control. “You’re not a good team player” — when rigid social expectations penalise alternative modes of communication. “You have a behavioural problem” — when institutional norms are built exclusively on the neurotypical blueprint.
The workplace: the office as a sensory battleground
Open-plan offices are a sensory catastrophe for neurodivergent people. But the problem goes beyond the physical environment. Performance standards are built on a neurotypical template: obligatory small talk, implicit communication, evaluations based on “presence” rather than outcomes.
The discrimination is documented and quantifiable: people who disclose an autism diagnosis receive 26% fewer expressions of interest from employers (Bury et al., 2020). Employers may alter working conditions to make it harder for autistic people to function, hoping they will resign.
Education: the child who “manages fine”
Long days in noisy, crowded environments, without demand-free recovery time, are a direct cause of burnout in neurodivergent children and young people. Teachers report that these students “manage fine” — but do not observe that “managing” costs three times more energy than it should.
Healthcare: the problem of the double empathy gap
Although 66% of autistic people have no associated intellectual disability, many clinicians lack adequate training to recognise autism in this population. The confusion between burnout and depression leads to prescriptions for behavioural activation — strategies that not only do not work but actively worsen autistic burnout. For a brain in burnout, behavioural activation is kryptonite.
And more alarmingly: healthcare environments themselves are sensorially hostile. Noisy, blindingly lit waiting rooms with unpredictable wait times discourage neurodivergent people from seeking the help they need.
◆ ◆ ◆
The Absence of Accommodations and the Illusion of Choice
“Take a break” — why it does not work
The advice “take a break” assumes that a break is available. For most neurodivergent people, it is not.
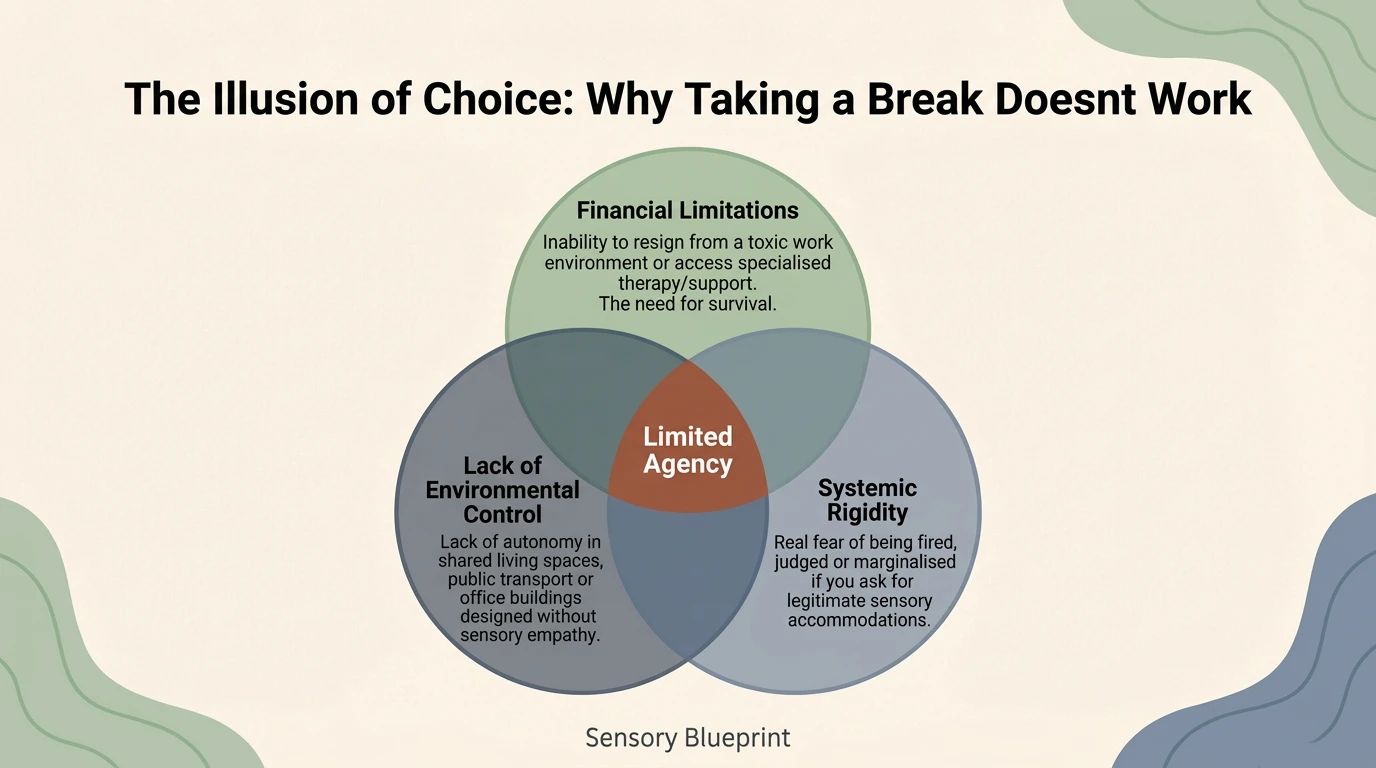
Financial constraints — The impossibility of leaving a toxic work environment or of accessing specialist therapies.
Systemic rigidity — The real fear of being dismissed, judged or marginalised for requesting legitimate sensory accommodations.
Lack of environmental control — You cannot control the lighting in the office, the noise in your flat, or the conditions on public transport.
Accommodations are not a luxury
Autism and ADHD are disabilities — often invisible, but real disabilities that require ongoing support.
These are not “special privileges”. They are the equivalent of wheelchair ramps — necessary, logical and beneficial for everyone. What in universal design is called the “curb-cut effect”: accommodations created for people with disabilities improve the experience for all.
The paradox is cruel: when neurodivergent people with high cognitive abilities ask for help, they are often met with disbelief. “But you seem completely normal” becomes a form of systemic gaslighting that invalidates the internal experience. The mask works so well that it becomes its own obstacle to obtaining support.
◆ ◆ ◆
The Cost of Conformity and Internalised Ableism

The voice that says “I should be able to”
The most insidious effect of social pressure does not come from outside — it comes from within. After years of repeated messages, the neurodivergent person internalises society’s voice: “I should be able to do this. Others manage. I’m just lazy. I’m exaggerating.”
This internalised ableism is one of the most powerful drivers of burnout, because it removes the last line of defence — the capacity to acknowledge one’s own limits. When you believe your limits are signs of weakness, you do not stop. And when you do not stop, your body stops for you.
Internalising neurotypical standards — Missed or late diagnoses lead to the belief that you are simply “lazy” or “weak”. Comparing yourself to non-autistic people and submitting to the same unrealistic expectations leads to chronic self-criticism.
Productivity pressure — We live in a world that measures human worth by productivity. “Rest and slowing down receive the unfortunate and incorrect label of ‘laziness’.”
People-pleasing as a trauma response — The tendency to please others is not politeness — it is often a fawn response (Pete Walker): compulsive submission and conflict avoidance through compliance.
The trauma of compliance-based therapies — Neurodivergent adults who experienced compliance-focused approaches in childhood lose their connection to their own internal sense and come to believe that their feelings and needs are unacceptable.
◆ ◆ ◆
What You Can Do: First Steps Towards Advocacy
If you have read this far and recognise yourself in these descriptions, you probably feel a mixture of validation and anger. Both are valid.
Personal advocacy
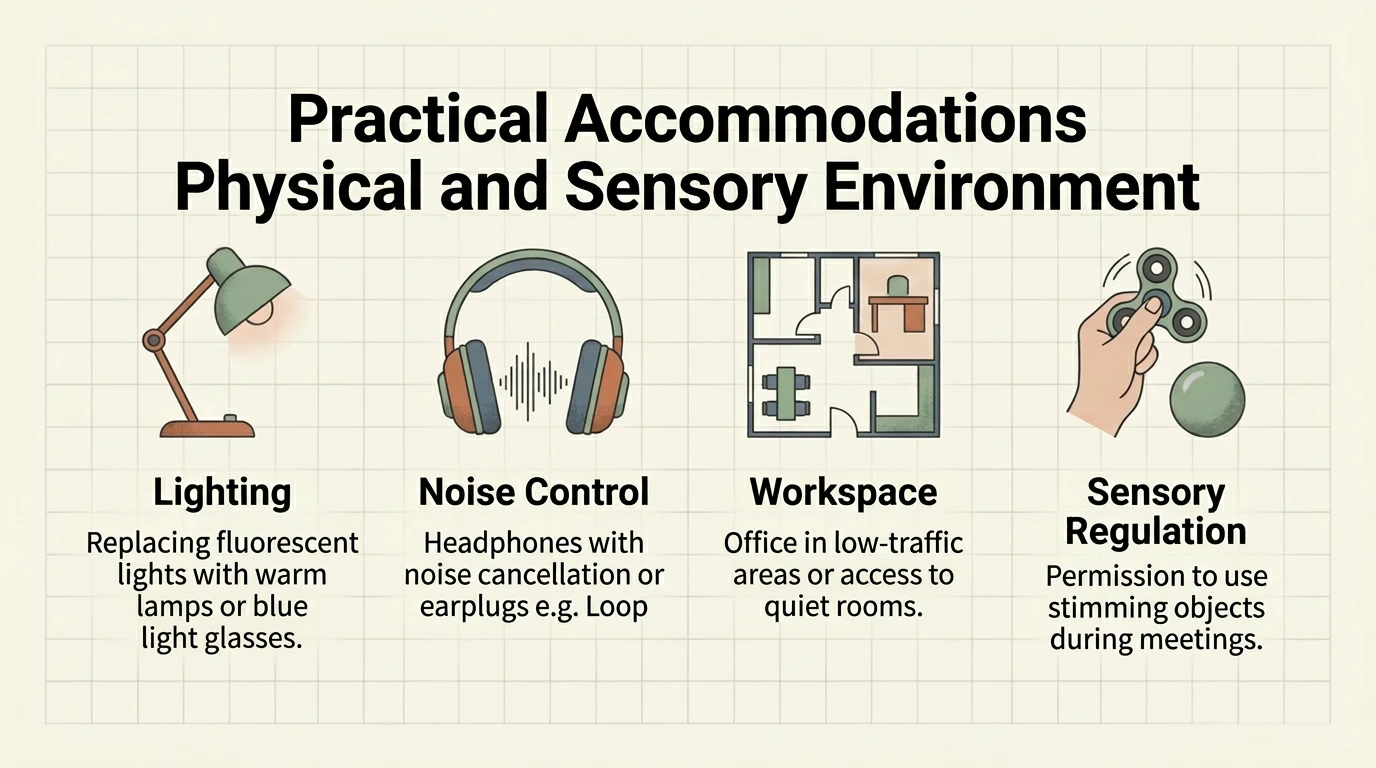
Selective disclosure — You do not have to disclose your diagnosis to everyone. But identify the people and contexts where disclosure can bring real accommodations. Prepare concrete language: “My nervous system processes sensory stimuli differently, which means I need…”
Create an accommodations plan — Identify the 3–5 adjustments that would make the most difference: written communication, processing time, controlled sensory environment, regular breaks, flexibility in scheduling.
Clear boundaries — Learn to say no without justification. “I cannot attend this meeting” is a complete sentence.
Challenge internalised ableism — Dismantle the inner voice that says “I should be able to work 40 hours like everyone else”. Neurotypical standards do not apply to a neurodivergent nervous system — just as visual standards do not apply to someone with myopia.
Community
Find your people — Online groups, local communities, spaces where you can exist without a mask. Belonging to a neurodivergent community is a significant protective factor against burnout (Botha & Frost, 2020).
Educating your support network — Family, friends and professionals need to understand the critical difference: isolation in burnout is strategic and adaptive. Withdrawal is the correct method — the opposite of “activation” used in depression.
Changing the narrative
Your burnout is not proof that you have failed. It is proof that you have tried too hard, for too long, in a system that did not provide the support you needed. Shifting responsibility from the individual to the context is not victimisation — it is scientific accuracy.
◆ ◆ ◆
What Comes Next in Part 4

We have explored how the environment overwhelms the senses and drains our batteries, while we ignore internal warning signals because of the absence of accommodations.
But what happens when the sensory system gives way completely? In Part 4 — “Interoception, Alexithymia and Executive Dysfunction” — we will explore the danger zone:
• Interoceptive differences — why we do not receive the “low battery” alert
• Alexithymia — when you know something is wrong but cannot name what
• Executive dysfunction — how sensory burnout destroys planning, working memory, speech
• Skills regression — why you can no longer do things you could do yesterday — and why this is not laziness but biological triage
The collapse seems “sudden” — but the signals were there all along. It was just that the internal dashboard was disconnected.
Ready to take the next step?
If what you have read resonates with you, you are not alone. Neurodivergent burnout is a real experience, validated by research — and there are neuro-affirmative strategies that can help.
Book an Initial Consultation →
Resources and support:
Telefonul sufletului (Romania): 0800 801 200 (free, 24/7)
Autistic community in Romania: suntautist.ro↗
ADHD resources in Romanian: despreadhd.ro↗
References
- Botha, M., & Frost, D. M. (2020). Extending the minority stress model. Society and Mental Health, 10(1), 20–34.
- Bury, S. M., et al. (2020). What language do autistic Australian adults prefer? J Autism Dev Disord, 50(11), 4082–4095.
- Cage, E., & Troxell-Whitman, Z. (2019). Reasons, contexts and costs of camouflaging. J Autism Dev Disord, 49(5), 1899–1911.
- Higgins, J. et al. (2021). Defining autistic burnout through experts by lived experience. Autism, 25(8), 2356–2369.
- Hull, L., et al. (2017). Social Camouflaging in Adults with ASC. J Autism Dev Disord, 47(8), 2519–2534.
- Mantzalas, J., et al. (2022). What is autistic burnout? Autism in Adulthood, 4(1), 52–65.
- Marco, E. J., et al. (2011). Sensory processing in autism: A review of neurophysiologic findings. Pediatric Research, 69(5 Pt 2), 48R–54R.
- Milton, D. E. M. (2012). The double empathy problem. Disability & Society, 27(6), 883–887.
- Raymaker, D. M., et al. (2020). Defining Autistic Burnout. Autism in Adulthood, 2(2), 132–143.
- Silvertant, E. (2024). Autistic Burnout: An Autistic Guide to Energy Management and Recovery. Jessica Kingsley Publishers.
- Walker, P. (2013). Complex PTSD: From Surviving to Thriving.

Specialising in neurodivergence — ADHD, Autism, AuDHD, and PDA. Working with adults navigating late diagnosis, burnout, and identity. 100% online.
Learn more about my approach →
Next Steps
If this resonated, here are practical ways to go deeper.

